You’re loading the dishwasher, or sitting in a work meeting, and suddenly it hits you. A flash of the affair. A mental image you didn’t ask for. Your chest tightens, your focus disappears, and you wonder if you’ll ever feel normal again. These moments don’t mean you’re broken or that healing isn’t happening. Intrusive thoughts are one of the most common and least talked about parts of recovering from betrayal, and the fact that you’re experiencing them says nothing about your strength or your progress. What matters is learning how to respond to them.
Table of Contents
- What are intrusive affair thoughts?
- Why intrusive thoughts happen: The science of rumination after betrayal
- How intrusive thoughts impact your daily life
- Evidence-based strategies to manage intrusive affair thoughts
- Creating a routine and environment that supports healing
- Recognizing progress and knowing when to seek more help
- Continue your recovery with structured support
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Intrusive thoughts are common | Most people recovering from infidelity struggle with sudden intrusive thoughts in daily life. |
| Science-backed strategies help | Therapies like CBT, EMDR, and ISTDP and practical daily techniques can reduce anxiety and rumination. |
| Routine and structure support healing | Daily schedules, self-care, and a supportive circle make managing these thoughts more effective. |
| Track improvement and seek help | Noticing progress is important, and reaching out for professional support is encouraged if needed. |
What are intrusive affair thoughts?
Intrusive thoughts are unwanted, repetitive, and distressing mental images, memories, or worries that appear without warning. In the context of affair recovery, they often take the form of mental replays of discovered details, imagined scenarios, or sudden waves of doubt and anger. You didn’t choose them, and you can’t simply decide to stop having them.
They occur because betrayal is a form of emotional trauma. Your brain’s stress response system, the same one designed to protect you from danger, gets activated by the shock of infidelity. It keeps scanning for threats, which is why intrusive thoughts after betrayal can closely resemble trauma responses seen in PTSD. Learning to stop obsessive thoughts starts with understanding why they happen in the first place.
Common triggers include:
- Moments of quiet or low stimulation, when the mind wanders
- Sensory reminders like a song, a smell, or a location
- Stress at work or in relationships
- Anniversaries or significant dates
- Seeing something that reminds you of the affair or the other person
“Intrusive rumination is a common feature of post-infidelity recovery and often linked to trauma responses.”
Understanding the infidelity trauma impact helps you stop blaming yourself for thoughts you didn’t invite.
Why intrusive thoughts happen: The science of rumination after betrayal
Rumination is the psychological term for repetitive negative thinking loops. It’s different from problem-solving. When you ruminate, your mind circles the same painful material without reaching resolution. After betrayal, this loop is driven by your brain’s threat detection system, which has been put on high alert.
The brain treats emotional betrayal similarly to physical danger. It keeps returning to the event, trying to make sense of it, looking for patterns, and searching for safety. This is not a flaw in your thinking. It’s a survival mechanism that hasn’t yet received the signal that the threat has passed.
Therapies like ISTDP significantly reduce rumination and self-doubt in those recovering from infidelity, which tells us these patterns are treatable, not permanent. Understanding the impact of infidelity trauma and processing emotional trauma are both key steps in breaking the loop.
| Feature | Rumination | Ordinary worry |
|---|---|---|
| Focus | Past events, replaying what happened | Future concerns, what might happen |
| Resolution | Rarely reaches a conclusion | Often leads to problem-solving |
| Emotional tone | Shame, anger, grief, confusion | Anxiety, caution |
| Control | Feels involuntary and intrusive | Feels more deliberate |
| Duration | Can last hours or days | Usually shorter and situational |
Pro Tip: Not every intrusive thought needs to be solved or analyzed. Simply noticing it, labeling it as “a thought,” and returning your attention elsewhere is often more effective than trying to reason your way out of it.
How intrusive thoughts impact your daily life
The ripple effects of intrusive affair thoughts go far beyond the moments they appear. They can quietly reshape your entire day.
Common daily disruptions include:
- Difficulty concentrating at work or during conversations
- Emotional swings that feel disproportionate to what’s happening around you
- Strained relationships with friends, family, or your partner due to withdrawal or irritability
- Avoidance behaviors, such as skipping places, events, or people that might trigger memories
- Sleep disruption, including difficulty falling asleep or waking with anxious thoughts
- Physical symptoms like tension headaches, fatigue, or a tight chest
Research shows that trauma therapies show effect sizes between .49 and .53 for reducing negative rumination and self-doubt, which confirms these are real, measurable symptoms, not just “being sensitive.” The effects of infidelity on anxiety are well documented, and managing obsessive thoughts is a skill that can be built over time.
Everyday situations can become unexpected triggers after infidelity. A restaurant you once visited together, a phrase your partner uses, even a particular time of day can pull you back into the pain. Recognizing these patterns is the first step toward regaining a sense of control.
Evidence-based strategies to manage intrusive affair thoughts
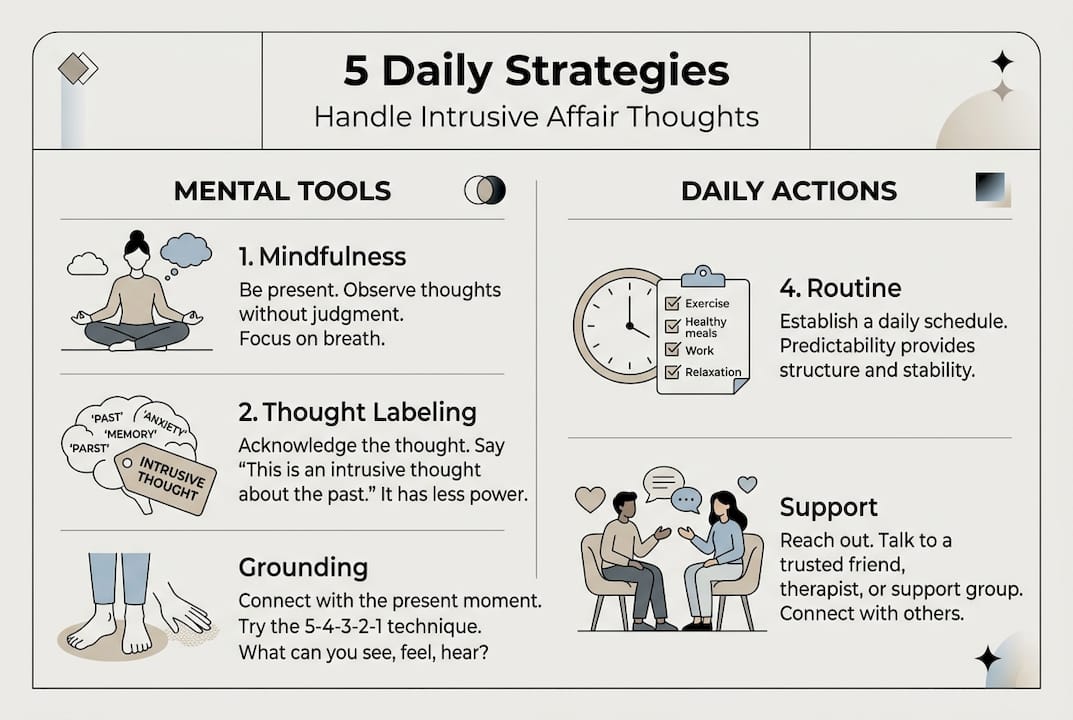
There is no single fix, but there are proven techniques that consistently help. The key is finding what works for you and practicing it regularly.
- Mindful noticing. When a thought appears, name it without judgment. Say to yourself, “I’m having the thought that…” This creates a small but important distance between you and the thought.
- Grounding exercises. Use your senses to anchor yourself to the present. Name five things you can see, four you can touch, three you can hear. This interrupts the rumination loop.
- Thought defusion. A technique from Acceptance and Commitment Therapy (ACT), this involves imagining your thoughts as leaves floating down a stream. You observe them without grabbing onto them.
- Diary logging. Write the thought down, note the time and trigger, and rate your distress from 1 to 10. Over weeks, you’ll see patterns and notice your distress scores dropping.
- Self-compassion response. When a thought hits, place a hand on your chest and say, “This is hard. I’m doing my best.” Research consistently shows self-compassion reduces emotional reactivity.
CBT, EMDR, and ISTDP each reduce intrusive thoughts in trauma recovery, with no significant difference in clinical outcomes between them. This means you have real options.
| Therapy | Key feature | Home-adapted practice |
|---|---|---|
| CBT | Challenges distorted thinking patterns | Thought diary, cognitive reframing |
| EMDR | Processes traumatic memories | Bilateral tapping, guided audio |
| ISTDP | Reduces emotional avoidance | Feeling journaling, body awareness |
Explore mindfulness for healing and coping after infidelity for more practical approaches. If you’re considering professional support, reviewing your therapy options can help you choose the right fit. You’ll also find specific tools to stop obsessive thoughts that complement these strategies.
Pro Tip: Consistency beats intensity every time. Five minutes of grounding practice every day will do more for you than an hour-long session once a week. Small, repeated actions rewire the brain’s response patterns.
Creating a routine and environment that supports healing
Strategies work best when they’re embedded in a structure that supports you. Without that structure, even the best techniques get forgotten under stress.
Here’s what a supportive daily routine can include:
- Scheduled check-in moments, such as a five-minute morning journal and an evening wind-down, to process emotions before they build up
- Regular physical movement, even a short walk, which reduces cortisol and interrupts rumination cycles
- Relaxation techniques like deep breathing or progressive muscle relaxation before bed
- Therapy appointments kept consistently, not just during crisis moments
- A support contact, one trusted person you can reach out to when thoughts feel overwhelming
- Limits on triggering interactions, including social media accounts or conversations that keep you stuck
Structured support combining social, professional, and self-guided elements consistently improves outcomes in infidelity recovery. Understanding the therapist’s role in recovery and actively processing emotional trauma are both part of building this structure.
Pro Tip: Prepare for triggered moments before they happen. Write a small reminder card that says something like, “This is a trigger. I am safe. I will use my grounding technique.” Keep it in your wallet or on your phone. Preparation defeats panic.
Self-forgiveness is also part of the structure. You will have bad days. You will sometimes react in ways you’re not proud of. That’s not failure. That’s recovery.
Recognizing progress and knowing when to seek more help
Progress in recovery rarely looks like a straight line upward. It looks more like a gradual shift in how quickly you recover after a difficult moment.
Signs that you are moving forward:
- Intrusive thoughts feel less intense, even if they still appear
- You recover your focus more quickly after a thought disrupts you
- You notice triggers before they fully take hold
- Emotional swings feel shorter in duration
- You can engage in daily activities with more consistency
These are real signs of healing, even when they feel small. ISTDP, CBT, and EMDR are all effective and can be adapted with a therapist or through self-help routines, which means your path forward has multiple valid options. Exploring individual or couples therapy can help you decide what level of support fits where you are right now.
Seek professional help if you experience persistent distress that doesn’t ease with self-help strategies, significant impairment in work or relationships, or any thoughts of harming yourself or others. These are not signs of weakness. They are signals that you need and deserve more targeted support. Your infidelity trauma recovery is worth investing in.
“Recovery is not linear; seeking help is a sign of strength, not failure.”
Continue your recovery with structured support
Managing intrusive thoughts is one piece of a larger healing process. When you have the right structure around you, recovery becomes less about white-knuckling through bad days and more about building a life that genuinely feels like yours again.

At aftertheaffair.uk, we’ve built resources specifically for where you are right now. The infidelity recovery checklist gives you a clear, step-by-step framework so you’re never guessing what to focus on next. If you’re thinking about rebuilding, the guide on relationship growth after infidelity walks you through what that actually looks like in practice. And if you’re supporting someone else through this, the guide for client healing offers professional-level insight in plain language. You don’t have to figure this out alone.
Frequently asked questions
Are intrusive affair thoughts normal in recovery?
Yes, intrusive thoughts after infidelity are very common and reflect a natural trauma response. Research confirms that betrayal closely resembles PTSD-type responses, which means your mind is reacting exactly as it’s designed to under extreme stress.
How long do intrusive affair thoughts usually last?
Duration varies from person to person, but with consistent evidence-based coping, most people notice a meaningful reduction in frequency and distress within several months. ISTDP reduces rumination significantly, which suggests that structured support accelerates the timeline.
What therapy is most effective for handling intrusive thoughts after infidelity?
CBT, EMDR, and ISTDP all show strong results, and no significant difference in clinical outcomes has been found between them. The best therapy is the one you’ll actually engage with consistently.
Should I seek professional help if intrusive thoughts won’t stop?
Yes. Persistent intrusive thoughts that interfere with daily functioning are a clear signal to consult a mental health professional. Structured professional support consistently improves recovery outcomes and is not a last resort but a smart early step.






